Karen Ann Quinlan had a cardiopulmonary
arrest in 1975 and died 10 years later, having
never regained consciousness. Her story prompted
a national debate about the appropriateness of
life-sustaining treatment in patients who are in
a persistent vegetative state and led to the
development of medicolegal guidelines for the
care of such patients.
Case Report : The clinical history and
findings are based on examination of the patient
by one of us, interviews with the attending
physicians, and a review of all relevant
documents, including medical and nursing
records. At 21 years of age, Karen Ann Quinlan
had a cardiopulmonary arrest after accidentally
ingesting a combination of prescription
sedatives and alcohol. When she was found, she
was unresponsive, apneic, pulseless, and
cyanotic with dilated pupils. She received
cardiopulmonary resuscitation. In the emergency
room, a pulse was present, but she was otherwise
unchanged and was placed on a ventilator. Within
the first hour after cardiopulmonary arrest,
spontaneous respirations and normal vital signs
had returned, but the patient remained
unresponsive to noxious stimuli and was
areflexic. During the first 12 hours, there was
sequential improvement, with the development of
pinpoint pupils and sluggish reaction to light,
upper-extremity flexion, toe inversion,
responsivity to pain, gag and cough reflexes,
spontaneous movement of all extremities, and
finally, opening of the eyes in response to
auditory stimuli. Aspiration pneumonia led to a
tracheostomy on the second day. Hypoxia occurred
transiently, with a low arterial partial
pressure of oxygen of 45 mm Hg. During the first
week after the arrest, stimulus-induced postural
patterns were seen, including flexion and
clenching of the hands, plantar flexion and
inversion of the feet, turning of the head to
the right, yawning, and grunting. With
intense stimulation, there was flexion of the
upper and lower extremities with marked spastic
rigidity, opisthotonos, and upward rolling of
the eyes. There was no response to threatening
gestures. Oculocephalic and oculovestibular
reflexes had returned to normal. All extremities
withdrew in response to a pinprick.
During the first six months after the arrest,
Quinlan had unequivocal sleep-wake cycles but
never showed signs of awareness of her
environment or cognitive function. During sleep
she rarely triggered the ventilator. Severe
contractures developed, and orofacial movements
(e.g., grimacing) dominated the arousal
responses in association with marked
diaphoresis, tachycardia, and tachypnea.
Quinlan's movements were never goal-directed but
always stereotypical and reproducible with a
given stimulus. Although she had the full range
of eye movement, her eyes moved randomly with
occasional disconjugate components, and she
never responded to stimuli with meaningful
extraocular movements. Quinlan had sufficient
primary motor competence to respond in a
meaningful fashion had any cognitive function
been intact, which buttressed the clinical
diagnosis of a persistent vegetative state, not
a locked-in state (i.e., conscious but with
severe paralysis, making vocal communication
impossible). A brain scan and bilateral carotid
and vertebral angiograms were unremarkable.
Electroencephalograms showed cortical activity
(predominantly low-voltage fast activity
[beta]) when the patient was awake. When
she appeared to be asleep, there was
intermittent low-voltage activity of 3 to 7 Hz ,
infrequent activity in the alpha range, and
occasional slower activity in the delta range.
During the first six months after the arrest,
the patient became severely cachectic, and her
weight stabilized at 32 to 34 kg (down from 52
kg) with hypercaloric feeding. Multiple lung,
bladder, and decubitus-ulcer infections were
treated.
During the second six months after the
arrest, Quinlan began to trigger the ventilator
more frequently while asleep, and she was weaned
from it over a period of a month, one year after
the arrest. Seizures (episodic twitching of the
extremities, mouth, and eyes for about 30
seconds) developed and were successfully treated
with phenytoin. A computed tomographic scan five
years after the arrest revealed cerebral and
cerebellar atrophy with generalized dilatation
of ventricular and cisternal systems. Fourteen
months after the arrest, Quinlan was transferred
to a nursing home where she remained in a
persistent vegetative state until her death nine
years later from overwhelming infection.
This report
describes the neuropathologic features of
Quinlan's brain.
Methods : The entire brain and spinal
cord were systematically sampled for histologic
examination. The brain stem and central cerebrum
were embedded en bloc and serially sectioned.
Three-dimensional computer reconstructions
helped visualize the topographic features of the
lesions.
Results : Contrary to expectation, the
most severe damage was not in the cerebral
cortex but in the thalamus, and the brain stem
was relatively intact. The neuropathological
findings included extensive bilateral thalamic
scarring, bilateral cortical scars primarily in
the occipital pole and parasagittal
parieto-occipital region, and bilateral damage
to cerebellar and focal-basal-ganglia regions.
The brain stem and basal forebrain and the
hypothalamic components of the ascending arousal
systems and brain-stem regions critical to
cardiac and respiratory control were undamaged.
The lesions were consistent with
hypoxia-ischemia after the cardiopulmonary
arrest.
Conclusions : Although the
neuropathological findings in the case of Karen
Ann Quinlan were complex, the disproportionately
severe damage in the thalamus as compared with
the cerebral cortex supports the hypothesis that
the thalamus is critical for cognition and
awareness and may be less essential for
arousal.
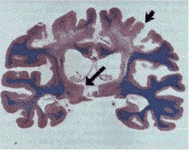
There was severe atrophy of the cerebral
cortex and underlying white matter in the border
zone of the anterior, middle, and posterior
cerebral arteries in the posterior frontal lobe
(short arrow). The thalamus (long arrow) was
severely atrophic bilaterally. (Hematoxylin and
eosin and Luxol fast blue.).